Indicators of safety
A survey published in the journal Infection Control and Hospital Epidemiology (tinyurl.com/pdjoesh) reveals 99% of polled surgeons suf- fered at least 1 needlestick in their careers. The problem, note the researchers, is that surgical glove punctures often go unnoticed during cases, meaning surgeons might be exposed to blood and associated infection risks without knowing it.
SURGEON SENSATION
It Takes Only 2 Weeks to Get a Feel for Double-Gloving
Your surgeons probably think that double-gloving reduces hand sensitivity and dexterity. “ Despite a large body of data supporting double-gloving, a major drawback of this intervention is the lack of surgeons’ acceptance,” write researchers Ramon Berguer, MD, and Paul Heller, MD, in the Journal of the American College of Surgeons (tinyurl.com/cd85fvl). The good news, the researchers say, is that it doesn’t take long for surgeons to start feeling acclimated to the decreased hand sensitivity associated with double-gloving.
“ Current underglove designs make double-gloving more comfortable and have led to improved 2-point discrimination — the ability of a surgeon to feel 2 points touching his skin,” says Dr. Berguer, who feels surgeons can fully adapt to double-gloving within 2 weeks of trying it for the first time.
— Daniel Cook
The researchers say glove puncture rates vary, although risks increase to as high as 70% during longer procedures as well as during surgeries requiring maximum effort in deep cavities and around
bones. They further note that research shows the risk of blood con- tact is decreased from 70% with single gloves to as low as 2% with double gloves, likely because the inner glove was shown to remain intact in up to 82% of cases.
To determine how much blood is transferred through single and double layers of gloves at the point of percutaneous injuries, the researchers stuck pork skin with automatic lancets, which simulated suture needlesticks. According to the findings, a mean volume of 0.064 L of blood is transferred in punctures at a depth of 2.4mm through 1 glove layer, compared with only 0.011 L of blood through
double-glove layers, which means the volume was reduced by a factor of 5.8.
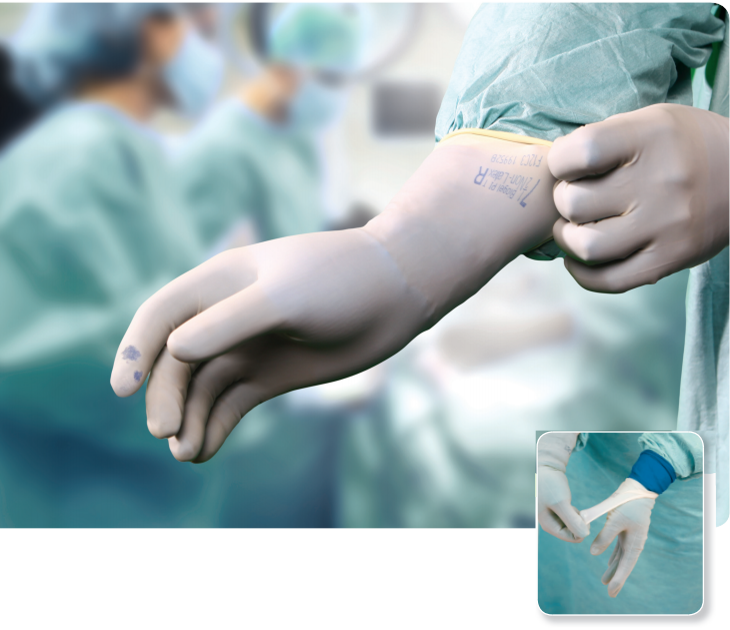
Notably, the double gloves used in the study included an indicator system: a green inner glove worn with a straw-colored outer glove. According to the researchers, all punctures of the gloves’ outer layers were clearly identifiable by the green coloring of the underglove showing at the puncture site. The color contrast reduces risk of blood exposure by alerting surgeons and staff to breaches that may have otherwise gone unnoticed.
“Double-gloving should be recommended for all surgical procedures and should be required for procedures performed on patients with known infections or patients who have not yet been tested for infections,” say the researchers. They also point out that while the protective effect of double-gloving is evident, it is not yet routine because of an alleged reduction in dexterity and sense of touch (for evidence to the contrary, see sidebar below).
Surgery ’s riskiest specialty
A report in Acta Orthopædica Belgica (tinyurl.com/qammhpz), official journal of the Belgian Society of Orthopedics and Traumatology, says glove perforation rates range from 10% in ophthalmology to 50% in general surgery. But the stress and strain of manipulating oscillating saws, metal instruments and implants during orthopedic procedures subject gloves to extreme shear force, putting orthopods at the great- est risk among surgical specialties, say the researchers.
In this study, the researchers assessed rates of glove perforations during major total hip and knee replacements and the more minor knee arthroscopies. They also examined how double-gloving impacted perforation rates and whether rates differed among sur- geons, their assistants and OR nurses.
The overall glove perforation rate was 15.8%, with a 3.6% rate during arthroscopies and a 21.6% rate duringjoint replacements. More than 72% of the breaches went unnoticed until after the procedures had
concluded. Only 3% of the inner gloves were jeopardized — none during arthroscopies — compared with 22.7% of the outer gloves.
Notably, only 4% of perforations recorded during major procedures involved both glove layers. A quarter of the 668 surgeons involved in the study suffered perforated gloves, which was significantly higher than the 8% of the 348 assistants and 512 nurses who suffered the same fate.
The researchers note that double-gloving in orthopedic procedures significantly reduces the incidence of perforation of inner gloves.
Although surgical personnel who scrub in properly lower their risks of contracting bloodborne diseases when gloves are perforated, they add, previous studies have shown bacteria cultures taken at perfora- tion sites have been positive about 10% of the time.
Post time: Jan-19-2024
